Neural indices of binaural hearing and spatial listening across the lifespan
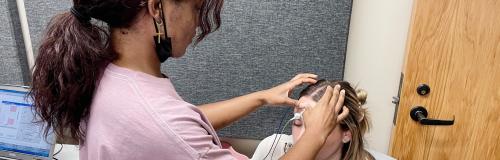
The human brain compares subtle acoustic differences between ears in a process known as binaural hearing. Binaural hearing allows us to perceptually segregate where sounds are coming from and to focus on those we are interested in while ignoring those we are not. The broad goals of this study are to understand how binaural hearing changes across the lifespan and to develop rapid and reliable ways to assess binaural hearing function clinically. The outcomes of this research may improve how we assess and treat patients with listening problems and/or hearing loss.
Examining the functional role of the auditory efferent system
Classic views of human hearing postulated that sound was detected by sensory receptors in the inner ear and delivered via neural impulses to the brain in a stepwise, ascending fashion. We now know that, in addition to the ascending auditory pathway, the brain sends neural signals back to the inner ear in an extensive descending pathway. The extent to which the descending auditory pathway helps us listen or sculpts the brain through neuroplastic changes is currently unclear. The goal of this project is to understand how processes like attention and learning commandeer the descending efferent pathway to help us hear. The outcomes of this research may elucidate which types of auditory training are most likely to improve auditory system function.
Objective measures of binaural sensitivity in cochlear implant users with bilateral acoustic hearing
Many cochlear implant recipients have preserved low frequency acoustic hearing following surgery. Evidence has shown that patients who use a combination of electric and acoustic stimulation (EAS) have better listening outcomes than those who rely exclusively on electric stimulation through the cochlear implant alone. Despite this, many patients who could use EAS do not. The goal of this study is to develop objective methods for assessing binaural hearing sensitivity in these patients to determine physiological biomarkers that predict EAS success. This project is led by the Cochlear Implant Lab at Vanderbilt University in collaboration with the TexAN Lab.

Improving Clinical Measures of Auditory Function
In many audiology clinics, the gold standard test battery for assessing hearing function includes a pure tone audiogram and basic evaluation of word recognition performance. Numerous studies have demonstrated that these tests may be poor predictors of which patients will struggle to hear in noisy environments. Further, it is often unclear which technological options (e.g., hearing aids, FM systems) should be considered for patients based on the outcomes of this test battery, especially when test results are putatively within normal limits. The goal of this project is to improve clinical assessment of auditory function to further characterize patients’ hearing abilities and guide them toward more appropriate treatment strategies. In this work, we use otoacoustic and electrophysiologic techniques to identify “subclinical” differences in auditory function and assess how these measures are related to listening performance. Outcomes of this study may improve clinical diagnostics by identifying patients with abnormal auditory function who would otherwise not be identified with the gold standard test battery.
We thank the following organizations for past and present support: